 |
||||||||||
Date: June 15, 2026
by Chaya Venkat
Related Alert:
No. 47 - Those Pesky Aches and Pains

Much of how our bodies work goes back to our evolution as naked apes on the plains of tropical Africa. Without the present day taboos on nudity, the full body surface of our ancestors was exposed to the sun each and every day, except when it was cloudy. Our modern lifestyle means we cover all except may be 5% of our skin surface, all except our faces and hands, less frequently our arms and legs. Unfortunately, evolution has designed us to need far more vitamin D (calciferol) than most of us get now — and a major source of vitamin D is its production in our skin as a result of UV exposure from sunlight. The relationship between vitamin D and sunlight is well documented. For example, submarine crews show a drop of approximately 40% in their blood levels of vitamin D metabolite after spending 2-3 months inside their under water steel home. New Pakistani immigrants to the colder and cloudier British climate have a whopping 80% drop in vitamin D metabolite one year after arriving in England.
It has been known for more than 60 years that people who get a lot of sun exposure are also likely to have fewer cancer deaths — that is, all except skin cancer. The direct link between squamous cell carcinoma and sun exposure has been known for a long time too. In fact putting these two facts together, a case of adding 2 + 2 and coming with 22, early researchers suggested that development of squamous cell carcinoma conferred immunity against all the other cancers! We know better now. Skin cancer has nothing to do with protecting us from other cancers. The same UV and sunlight that causes skin cancer also helps make vitamin D in our skin and vitamin D is a powerful cancer preventive agent.
It is now rare for us to spend a lot of time in full strength sunlight, without clothes or sun protection getting in the way. And rightly so! If you have not read the recent article "Dying to Get a Tan?" on our website, today may be a good day to read it. The risk of squamous cell carcinoma is much higher in CLL patients and if it develops, it is likely to be of a more aggressive and hard-to-treat variety. There is no escaping this — for CLL patients, there are serious risks associated with sun exposure and aggressive skin cancers. Sounds like one of life's classic damned-if-you-do and damned-if-you-don't type of choices, right? Not quite. For a change, there is a simple, inexpensive and downright obvious solution. It is possible to eat your cake and have it too. The answer to getting enough vitamin D without getting too much sun (and thereby running the risk of skin cancer) is swallowing a capsule with the right level and right type of vitamin D.
Vitamin D is a powerful hormone and its function in the endocrine system is complex. I will not bore you with the details. But this much you should know: vitamin D is metabolized by the liver and kidneys to form something called 25-hydroxyvitamin D (25(OH)D, for short). It is now clear that vitamin D influences many organs including the intestines, bone, kidneys, pancreas, B cells, pituitary gland, breast tissue, placenta, lymphocytes, keratinocytes, colon, prostate and a few more that I might have overlooked. It is a serious player in many cancers. Much of the health benefits of sunlight is associated with increased levels of this potent inhibitor of cancer cell proliferation.
Let's get some units straight in our heads before we proceed. Vitamin D is measured in micrograms (the symbol is "µg", the Greek letter mu indicating "micro" or one-milliionth), which is one millionth of a gram. Another common measure is the International Unit (symbol is "IU"). Scientists use both units of measurement and it can get confusing. Here is the simple conversion: 1 µg of Vitamin D = 40 IU. You are more likely to see the IU units on bottles of multivitamins. I will give both units in the rest of this review, so that you can pick the one you want to use.
With a few exceptions, there is little or no vitamin D in the kind of foods that humans normally eat, unless they are artificially supplemented. The conventional wisdom used to be that occasional exposure of the face and hands to sunlight is "sufficient" for vitamin D production. However, now there is solid evidence that the amount of Vitamin D produced by 5% skin exposure would leave more than half of the population "Vitamin D insufficient". Several researchers have found that in the homebound American elderly, the mean vitamin D intake was 13 µg (520 IU) per day. When this is converted to the active metabolite 25(OH)D in the body, this amount of vitamin D puts most people into the "vitamin D insufficient" category.
Some of the abstracts I have attached document the way the adult Recommended Daily Allowance (RDA) for vitamin D has been set in this country and elsewhere. The current adult RDA for Vitamin D approximates half the amount in a teaspoon of cod-liver oil. Our modern day RDA is based pretty much on that 19th-century folk remedy. In England, an adult requirement of only 2.5 µg (100 IU)/day was justified on the basis of 7 adult women with severe nutritional lack of vitamin D, whose bones showed a response when given this amount. These were hardly a representative group of adults, and in any case the decision was made on the basis of just reversing the extreme bone decay, not the level required for good general health. The adult RDA of 5 µg (200 IU)/d was described as a "generous allowance" in the 1989 version of American recommended intakes. While the American adult RDA for vitamin D has remained unchanged since the 1960s, it has been newly revised for people older than 70 years — it is now 3-fold higher than the standard RDA.
The required vitamin D fortification of milk, orange juice and a few other foods over the past several decades, coupled with the general use of vitamin D supplements in children, has eliminated diseases such as rickets associated with severe vitamin D deficiency. But the same approach has not succeeded in preventing a milder form of the problem, vitamin D insufficiency. It has now been well documented that significant subsets of North Americans have lower levels of 25(OH)D, the Vitamin D metabolite, than necessary to maintain good health. There is a rapidly growing body of evidence that one of the downsides of not having enough Vitamin D is the increased risk of many types of cancer, a situation that can be easily corrected with Vitamin D supplements.
Another area of intense interest as the general age of our populations increase is that increasing blood concentrations of 25(OH)D from 50 nmol/L to 80 nmol/L improves calcium absorption efficiency by nearly two-thirds and reduces osteoporotic fracture risk by one-third. We are conditioned to think of osteoporosis as a problem faced by post-menopausal women. It is not quite that simple. All of us, men and women, are at risk of thinning and brittle bones as we age, especially if we lead sedentary lives without weight bearing exercise. If on top of that we add the risk factor of chemotherapy, especially with corticosteroid drugs such as prednisone, justly famous for their side-effect of leaching calcium out of bones, you can see why this is an important issue for CLL patients.
So what is the problem, you ask, why not load everyone to the gills with Vitamin D? In simple terms, mega doses of Vitamin D can cause hypercalcemia, which in layperson terms means there is too much free calcium (Ca2+) in the blood. Most of us obsess over the monthly CBC, going crazy over each dip and up tick in the lymphocyte numbers, instead of doing the sensible thing and look for clear trends over time by charting the data. There is a certain amount of "noise" in any of this data, especially if the CBC is done at different labs. You may not get a "Blood Electrolytes" (also called "composite metabolic panel" by some labs) work-up as often as you get your CBC checked out but I think it is important to get this done, too, on a regular basis. Our charts template has a sheet on it for monitoring the electrolyte information. One of the items on that chart, namely your calcium levels, is worth monitoring.
The calcium ion (Ca2+) concentration is controlled by two hormones, parathyroid hormone (PTH) and vitamin D. PTH keeps tabs on calcium concentration on a minute by minute basis. When the concentration drops, this hormone triggers the release of calcium from the stored reserves in your kidneys as well as your bones. It also converts vitamin D to its active form, which helps your gut absorb more calcium from the food you eat.
Hypercalcemia is a dangerous and life-threatening disorder in cancer patients. Roughly 10% - 20% of all patients with solid tumors as well as blood cancers (particularly multiple myeloma) have hypercalcemia, a condition in which the calcium level in blood serum is way too high. Left untreated, hypercalcemia quickly becomes life threatening. In fact, withholding intervention to correct hypercalcemia is one of the ways in which hospitals and doctors honor end-of-life wishes of patients and their families. Here is a quote from the NCI monograph on hypercalcemia:
"When a patient has a refractory, widely disseminated malignancy for which specific therapy is no longer being pursued, the patient may want to consider withholding therapy for hypercalcemia. For patients or family who have expressed their wishes regarding end-of-life issues, this may represent a preferred timing and/or mode of death (as compared to a more prolonged death from advancing metastatic disease). This option is best considered long before the onset of severe hypercalcemia or other metabolic abnormalities that impair cognition, so that the patient may be involved in the decision-making".
I hope you have now clearly understood that hypercalcemia is not something to take lightly. Left untreated, severe hypercalcemia quickly leads to coma and death. However, while hypercalcemia is clearly of concern if one is taking too much Vitamin D, published cases of vitamin D toxicity with hypercalcemia typically involve the intake of more than 1,000 µg (40,000 IU)/day. Most nutritionists and researchers appear to agree that supplementation of Vitamin D with 25 µg (1,000 IU)/day poses little risk of hypercalcemia. It is unfortunate this level of supplementation has been avoided even though the weight of evidence shows that this is a safe level, likely to provide some protection against cancers of many kinds.
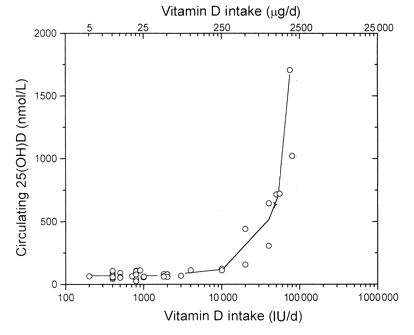
Dose response for vitamin D intake versus
final serum level of 25(OH)D concentration
(Vitamin D Supplementation - R. Vieth)
The graph above shows the relationship between the amount of Vitamin D intake and the amount of the metabolite 25(OH)D measured in blood serum. As you can see, the level of 25(OH)D does not increase sharply until the Vitamin D intake exceeds about 10,000 IU per day. This is well below the threshold level — 1,000μg (40,000 IU) — where hypercalcemia is observed.
GPs have noticed a strange connection between northern latitudes, winter times and the general health of their patients. Besides the psychological strain of living during the gloomy winter months when the sky is overcast, daylight hours are short and it is too cold to go out into the sunlight anyway, there is also a direct correlation between sun exposure of skin, vitamin D levels and good health. The abstract below from Minnesota spells it out: their cold winters and short days do take a toll.
Minn Med. 2026 Jan;86(1):43-5.
Vitamin D--the steroid hormone prescription for every patient.
Plotnikoff GA.
University of Minnesota, Minneapolis, MN
Physicians in the United States rarely screen for hypovitaminosis D and rarely prescribe vitamin D, even when medically indicated. This is of particular concern in Minnesota. The sun's intensity at Minnesota's latitudes limits vitamin D production, at best, to March through October. A variety of lifestyle situations, including long work hours, may preclude adequate sun exposure. Additionally, people of Northern European background may avoid sun exposure to reduce risk of skin cancer and premature aging. And people of Asian and African heritage may not have sufficient vitamin D production due to increased skin pigmentation. This brief article summarizes key points regarding the importance of vitamin D, including its action as a steroid hormone and its role in cancer, hypertension, and autoimmune disease as well as in perinatal and prenatal health. The potential benefit of hypovitaminosis D screening and vitamin D supplementation is discussed, as are the populations most likely to need screening and supplementation.
PMID: 12585559
____________
The two abstracts below by Vieth, et al., (you can and should click on the links provided, to read the full text articles for free) are very extensive and detailed. They will provide you with a great deal of the background information, and even more important, they will be useful documents to have when/if you decide to pick up this topic as a discussion item with your GP or oncologist. Both the articles also have a wealth of references, if you wish to research this subject further.
Article from the American Journal of Clinical Nutrition
Am J Clin Nutr. 1999 May;69(5):842-56.
Vitamin D supplementation, 25-hydroxyvitamin D concentrations, and safety.
Vieth R.
Department of Laboratory Medicine and Pathobiology, University of Toronto, Mount Sinai Hospital, Ontario, Canada.
For adults, the 5-microg (200 IU) vitamin D recommended dietary allowance may prevent osteomalacia in the absence of sunlight, but more is needed to help prevent osteoporosis and secondary hyperparathyroidism. Other benefits of vitamin D supplementation are implicated epidemiologically: prevention of some cancers, osteoarthritis progression, multiple sclerosis, and hypertension. Total-body sun exposure easily provides the equivalent of 250 microg (10000 IU) vitamin D/d, suggesting that this is a physiologic limit. Sailors in US submarines are deprived of environmentally acquired vitamin D equivalent to 20-50 microg (800-2000 IU)/d. The assembled data from many vitamin D supplementation studies reveal a curve for vitamin D dose versus serum 25-hydroxyvitamin D [25(OH)D] response that is surprisingly flat up to 250 microg (10,000 IU) vitamin D/d. To ensure that serum 25(OH)D concentrations exceed 100 nmol/L, a total vitamin D supply of 100 microg (4000 IU)/d is required. Except in those with conditions causing hypersensitivity, there is no evidence of adverse effects with serum 25(OH)D concentrations <140 nmol/L, which require a total vitamin D supply of 250 microg (10,000 IU)/d to attain. Published cases of vitamin D toxicity with hypercalcemia, for which the 25(OH)D concentration and vitamin D dose are known, all involve intake of greater than or equal to 1000 microg (40,000 IU)/d. Because vitamin D is potentially toxic, intake of >25 microg (1000 IU)/d has been avoided even though the weight of evidence shows that the currently accepted, no observed adverse effect limit of 50 microg (2000 IU)/d is too low by at least 5-fold.
PMID: 10232622
____________
Article from the American Journal of Clinical Nutrition
Am J Clin Nutr. 2026 Feb;73(2):288-94.
Efficacy and safety of vitamin D3 intake exceeding the lowest observed adverse effect level.
Vieth R, Chan PC, MacFarlane GD.
Mount Sinai Hospital, Toronto, Ontario, Canada.
BACKGROUND: The Food and Nutrition Board of the National Academy of Sciences states that 95 microg vitamin D/d is the lowest observed adverse effect level (LOAEL).
OBJECTIVE: Our objective was to assess the efficacy and safety of prolonged vitamin D3 intakes of 25 and 100 microg (1000 and 4000 IU)/d. Efficacy was based on the lowest serum 25-hydroxyvitamin D [25(OH)D] concentration achieved by subjects taking vitamin D3; potential toxicity was monitored by measuring serum calcium concentrations and by calculating urinary calcium-creatinine ratios.
DESIGN: Healthy men and women (n = 61) aged 41 +/- 9 y (mean +/- SD) were randomly assigned to receive either 25 or 100 microg vitamin D3/d for 2-5 mo, starting between January and February. Serum 25(OH)D was measured by radioimmunoassay.
RESULTS: Baseline serum 25(OH)D was 40.7 +/- 15.4 nmol/L (mean +/- SD). From 3 mo on, serum 25(OH)D plateaued at 68.7 +/- 16.9 nmol/L in the 25-microg/d group and at 96.4 +/- 14.6 nmol/L in the 100-microg/d group. Summertime serum 25(OH)D concentrations in 25 comparable subjects not taking vitamin D3 were 46.7 +/- 17.8 nmol/L. The minimum and maximum plateau serum 25(OH)D concentrations in subjects taking 25 and 100 microg vitamin D3/d were 40 and 100 nmol/L and 69 and 125 nmol/L, respectively. Serum calcium and urinary calcium excretion did not change significantly at either dosage during the study.
CONCLUSIONS: The 100-microg/d dosage of vitamin D3 effectively increased 25(OH)D to high-normal concentrations in practically all adults and serum 25(OH)D remained within the physiologic range; therefore, we consider 100 microg vitamin D3/d to be a safe intake.
PMID: 11157326
____________
Below is an article that brings the whole issue of vitamin D into sharper focus. Did you know that vitamin D is quite cytotoxic to CLL cells? In fact, they are busy researching molecules that are very similar to vitamin D, such as EB1089 below, in the hope of finding one that has as much therapeutic value as the normal Vitamin D, but less likely to cause hypercalcemia.
I am sure you have all seen anecdotal stories on the various internet chat rooms: a CLL patient living in one of our more northern states goes down to Florida every winter, to take advantage of the warmer and sunnier climate as well as daily game of golf. Presto! Every year his CLL counts stop rising or even fall back a little over this period. Perhaps there are other reasons for this, but one reason that suggests itself is that the patient in question has a chronic case of Vitamin D insufficiency, which is temporarily corrected when he gets a lot more sun over the winter months playing golf. Now, would it not be grand if he could get the same effect year round, by the simple act of taking a Vitamin D capsule? Something to think about. Unfortunately, and I am quoting from the Mayo abstract, "Physicians in the United States rarely screen for hypovitaminosis D and rarely prescribe vitamin D, even when medically indicated". If your healthcare provider falls into this category, it is probably important for you to get a little proactive.
Blood. 2026 Apr 1;101(7):2454-60. Epub 2026 Nov 21.
The vitamin D3 analog EB1089 induces apoptosis via a p53-independent mechanism involving p38 MAP kinase activation and suppression of ERK activity in B-cell chronic lymphocytic leukemia cells in vitro.
Pepper C, Thomas A, Hoy T, Milligan D, Bentley P, Fegan C.
Department of Haematology, Llandough Hospital, Penarth, Vale of Glamorgan, United Kingdom.
EB1089, a novel vitamin D3 analog, has been shown to have cytotoxic and antiproliferative properties in a variety of malignant cells. However, its potential as a treatment for B-cell chronic lymphocytic leukemia (B-CLL) has not been evaluated. EB1089 induced apoptosis in all of the 102 B-CLL samples tested with a mean LD(50) (the concentration of EB1089 required to kill 50% of cells) value (+/- SD) of 2.1 x 10(-8) M (+/- 1.4 x 10(-8) M). Furthermore, no significant difference was found in the cytotoxicity of EB1089 in B-CLL samples from previously treated and untreated patients (P =.1637). Induction of apoptosis was associated with a reduction in Bcl-2 and Mcl-1 protein expression, but this was evident only in the apoptotic cells. In contrast, the expression of Bax, p21, and p53 was not altered in the viable or apoptotic cells from either B- or T-lymphocyte lineages. EB1089-induced apoptosis was preceded by activation of p38 mitogen-activated protein (MAP) kinase and suppression of extracellular signal-regulated kinase (ERK) activity, and this was associated with downstream activation of caspase-3. The pancaspase inhibitor (Z-VAD-FMK) and the caspase-9 inhibitor (Z-LEHD-FMK) were able to partially abrogate the apoptotic effects of EB1089 but did not affect the phosphorylation of p38 MAP kinase or the suppression of ERK. The B-CLL cells in the study were shown to highly express vitamin D receptor, but an additional receptor-independent mechanism of cell killing cannot be ruled out at this stage. These findings show that EB1089 is a potent apoptosis-inducing agent in B-CLL cells and may be useful in the treatment of B-CLL patients, particularly those with p53 mutations or drug-resistant disease.
PMID: 12446453
____________
The abstracts I have discussed above, as well as several others attached below are from top-rated journals, authors from some of our most prestigious medical research facilities. There are dozens more, I just had to put some limit on the length of this review. Vitamin D has the potential to play a significant role in remission maintenance, or even delaying the day when first therapy becomes inevitable. It is important to do your homework, and go about it in a cautious and pragmatic manner. Here are a set of action items I strongly recommend:
N Engl J Med. 1998 Mar 19;338(12):777-83.
Hypovitaminosis D in medical inpatients.
Thomas MK, Lloyd-Jones DM, Thadhani RI, Shaw AC, Deraska DJ, Kitch BT, Vamvakas EC, Dick IM, Prince RL, Finkelstein JS.
Endocrine Unit, Massachusetts General Hospital and Harvard Medical School, Boston MA 02114
BACKGROUND: Vitamin D deficiency is a major risk factor for bone loss and fracture. Although hypovitaminosis D has been detected frequently in elderly and housebound people, the prevalence of vitamin D deficiency among patients hospitalized on a general medical service is unknown.
METHODS: We assessed vitamin D intake, ultraviolet-light exposure, and risk factors for hypovitaminosis D and measured serum 25-hydroxyvitamin D, parathyroid hormone, and ionized calcium in 290 consecutive patients on a general medical ward.
RESULTS: A total of 164 patients (57 percent) were considered vitamin D-deficient (serum concentration of 25-hydroxyvitamin D, < or = 15 ng per milliliter), of whom 65 (22 percent) were considered severely vitamin D-deficient (serum concentration of 25-hydroxyvitamin D, <8 ng per milliliter). Serum 25-hydroxyvitamin D concentrations were related inversely to parathyroid hormone concentrations. Lower vitamin D intake, less exposure to ultraviolet light, anticonvulsant-drug therapy, renal dialysis, nephrotic syndrome, hypertension, diabetes mellitus, winter season, higher serum concentrations of parathyroid hormone and alkaline phosphatase, and lower serum concentrations of ionized calcium and albumin were significant univariate predictors of hypovitaminosis D. Sixty-nine percent of the patients who consumed less than the recommended daily allowance of vitamin D and 43 percent of the patients with vitamin D intakes above the recommended daily allowance were vitamin D-deficient. Inadequate vitamin D intake, winter season, and housebound status were independent predictors of hypovitaminosis D in a multivariate model. In a subgroup of 77 patients less than 65 years of age without known risk factors for hypovitaminosis D, the prevalence of vitamin D deficiency was 42 percent.
CONCLUSIONS: Hypovitaminosis D is common in general medical inpatients, including those with vitamin D intakes exceeding the recommended daily allowance and those without apparent risk factors for vitamin D deficiency.
PMID: 9504937
___________
Article from the American Journal of Clinical Nutrition
Am J Clin Nutr. 2026 Nov;78(5):912-9.
Long-latency deficiency disease: insights from calcium and vitamin D.
Heaney RP.
Creighton University, Omaha, NE 68131
Nutrient intake recommendations and national nutritional policies have focused primarily on prevention of short-latency deficiency diseases. Most nutrient intake recommendations today are based on prevention of the index disease only. However, inadequate intakes of many nutrients are now recognized as contributing to several of the major chronic diseases that affect the populations of the industrialized nations. Often taking many years to manifest themselves, these disease outcomes should be thought of as long-latency deficiency diseases. Sometimes they come about by the same pathophysiologic mechanism that produces the index disease, but sometimes the mechanisms are completely different. Well-documented examples of both short- and long-latency deficiency states involving calcium and vitamin D are described briefly. Then, the insights derived from these nutrients are tentatively applied to folic acid. Discerning the full role of nutrition in long-latency, multifactorial disorders is probably the principal challenge facing nutritional science today. The first component of this challenge is to recognize that inadequate intakes of specific nutrients may produce more than one disease, may produce diseases by more than one mechanism, and may require several years for the consequent morbidity to be sufficiently evident to be clinically recognizable as "disease." Because the intakes required to prevent many of the long-latency disorders are higher than those required to prevent the respective index diseases, recommendations based solely on preventing the index diseases are no longer biologically defensible.
PMID: 14594776
____________
Article from the American Journal of Clinical Nutrition
Am J Clin Nutr. 2026 Mar;79(3):362-71.
Vitamin D: importance in the prevention of cancers, type 1 diabetes, heart disease, and osteoporosis.
Holick MF.
Vitamin D, Skin, and Bone Research Laboratory, Section of Endocrinology, Diabetes, and Nutrition, Department of Medicine, Boston University School of Medicine, Boston, MA 02118-2394
The purpose of this review is to put into perspective the many health benefits of vitamin D and the role of vitamin D deficiency in increasing the risk of many common and serious diseases, including some common cancers, type 1 diabetes, cardiovascular disease, and osteoporosis. Numerous epidemiologic studies suggest that exposure to sunlight, which enhances the production of vitamin D(3) in the skin, is important in preventing many chronic diseases. Because very few foods naturally contain vitamin D, sunlight supplies most of our vitamin D requirement. 25-Hydroxyvitamin D [25(OH)D] is the metabolite that should be measured in the blood to determine vitamin D status. Vitamin D deficiency is prevalent in infants who are solely breastfed and who do not receive vitamin D supplementation and in adults of all ages who have increased skin pigmentation or who always wear sun protection or limit their outdoor activities. Vitamin D deficiency is often misdiagnosed as fibromyalgia. A new dietary source of vitamin D is orange juice fortified with vitamin D. Studies in both human and animal models add strength to the hypothesis that the unrecognized epidemic of vitamin D deficiency worldwide is a contributing factor of many chronic debilitating diseases. Greater awareness of the insidious consequences of vitamin D deficiency is needed. Annual measurement of serum 25(OH)D is a reasonable approach to monitoring for vitamin D deficiency. The recommended adequate intakes for vitamin D are inadequate, and, in the absence of exposure to sunlight, a minimum of 1000 IU vitamin D/d is required to maintain a healthy concentration of 25(OH)D in the blood.
PMID: 14985208
____________
CMAJ. 2026 Jun 11;166(12):1517-24.
Vitamin D insufficiency in a population of healthy western Canadians.
Rucker D, Allan JA, Fick GH, Hanley DA.
Department of Medical Science, University of Calgary, Alta.
BACKGROUND: People with low levels of vitamin D and its metabolites are at increased risk for osteoporotic fractures. We wished to ascertain levels of vitamin D in a representative sample of adult western Canadians, to help assess the level of risk. We evaluated the prevalence of vitamin D insufficiency, defined as 25-hydroxyvitamin D [25(OH)D] less than 40 nmol/L, and seasonal variations in 25(OH)D, parathyroid hormone and related biochemical indices in a community-dwelling population of healthy Canadians living in Calgary (latitude 51 degrees 07'N).
METHODS: During calendar year 1999, we collected fasting overnight blood samples every 3 months from 60 men and 128 women (age range 27 to 89 years) who had volunteered to participate in another study. We used commercial radioimmunoassay kits to measure calciotrophic hormones and other biochemical indices. Regression models for longitudinal data were used to assess the effect of season and other potential predictors on individual parameters.
RESULTS: For a total of 64 participants (34%), vitamin D insufficiency, defined as 25(OH)D less than 40 nmol/L, was recorded at least once out of the 4 sampling times. After adjustment for age, body mass index and holiday travel, we observed the anticipated rise in serum 25(OH)D from a mean of 57.3 (standard deviation [SD] 21.3) nmol/L in the winter to 62.9 (SD 28.8) nmol/L in spring (p = 0.001) and 71.6 (SD 23.6) nmol/L in summer (p < 0.001), with a subsequent decline to 52.9 (SD 17.2) nmol/L in the fall (p = 0.008). The anticipated inverse relation between 25(OH)D and parathyroid hormone was not consistently observed: after adjustment for age, sex, body mass index and serum calcium, serum levels of parathyroid hormone did decrease significantly, from 39.5 (SD 18.8) ng/L in winter to 36.3 (SD 17.8) ng/L in summer (p = 0.001), but they continued to decline to 34.5 (SD 17.3) ng/L in the fall (p < 0.001). There was no association between 25(OH)D and parathyroid hormone (p = 0.21).
INTERPRETATION: We documented a high prevalence of vitamin D insufficiency, which warrants consideration of dietary vitamin D supplementation.
________
 Enter Keywords: |
———
Disclaimer: The content of this website is intended for information only and is NOT meant to be medical advice. Please be sure to consult and follow the advice of your doctors on all medical matters.
Copyright Notice:
Copyright © 2026-2007 CLL Topics, Inc. All Rights Reserved.
All materials contained on this site are protected by United States copyright law and may not be reproduced, distributed, transmitted, displayed, published or broadcast without the prior written permission of CLL Topics, Inc. You may not alter or remove any trademark, copyright or other notice from copies of the content.
However, you may download and print material from CLLTopics.org exclusively for your personal, noncommercial use.
———
